 We do not “get” fungal infections, the fungus is already there. You may not be aware that we ALL carry fungal elements on our skin naturally. The saying that fungus is “all among us” is actually true. Candida albicans is the most common fungal organism residing quite comfortably on our skin, mouth, gastrointestinal and vaginal areas. When provided the right environment, the organism multiplies uncontrollably leading to an infection. The right environment involves a shift in the natural bacterial flora due to antibiotics, poor hygiene, contact sports such as wrestling, compromised immune system following an illness, chemotherapy, HIV or exposure to frequent wet conditions. The yeast infection on the skin manifests as red, itchy welts that may drain a clear or white-yellow substance. Nail infections may become painful, red and swollen impeding normal manual dexterity.
We do not “get” fungal infections, the fungus is already there. You may not be aware that we ALL carry fungal elements on our skin naturally. The saying that fungus is “all among us” is actually true. Candida albicans is the most common fungal organism residing quite comfortably on our skin, mouth, gastrointestinal and vaginal areas. When provided the right environment, the organism multiplies uncontrollably leading to an infection. The right environment involves a shift in the natural bacterial flora due to antibiotics, poor hygiene, contact sports such as wrestling, compromised immune system following an illness, chemotherapy, HIV or exposure to frequent wet conditions. The yeast infection on the skin manifests as red, itchy welts that may drain a clear or white-yellow substance. Nail infections may become painful, red and swollen impeding normal manual dexterity.Fungal organisms thrive in damp, dark and warm environments. Nail salons, tanning beds, hot tubs, sauna and locker room floors are covered with these opportunistic creatures hungry for a new adventure between our toes and crevices.
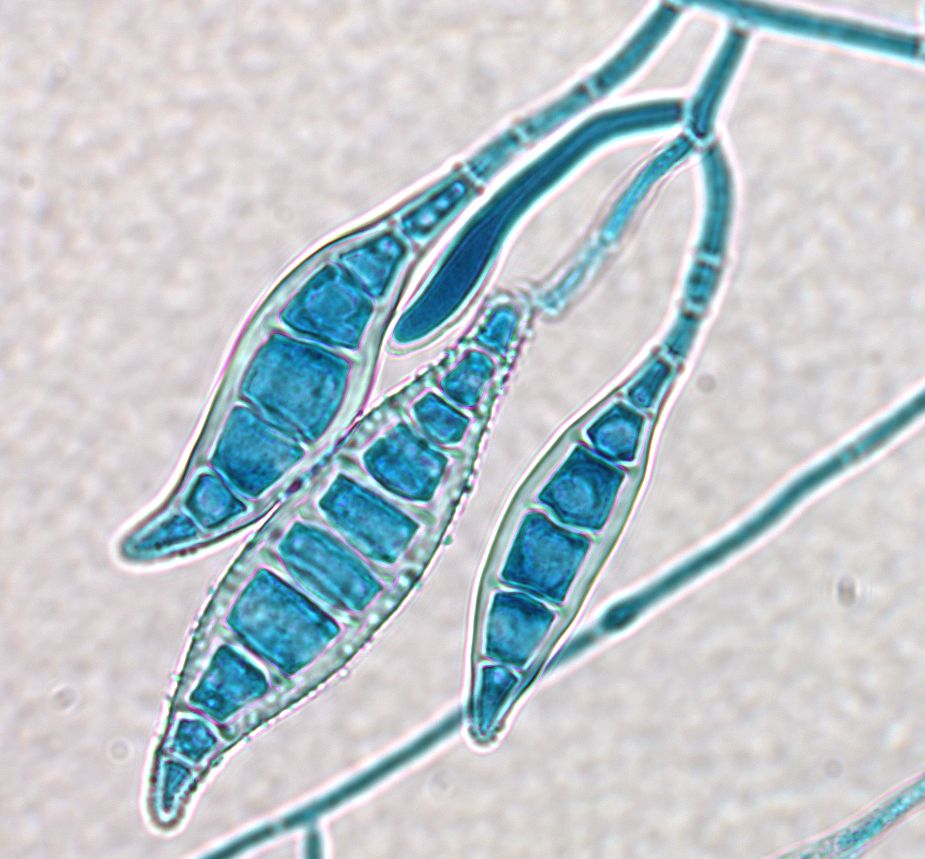
Dermatophytes are fungi that live on dead tissue, such as the nails and dead skin cells.
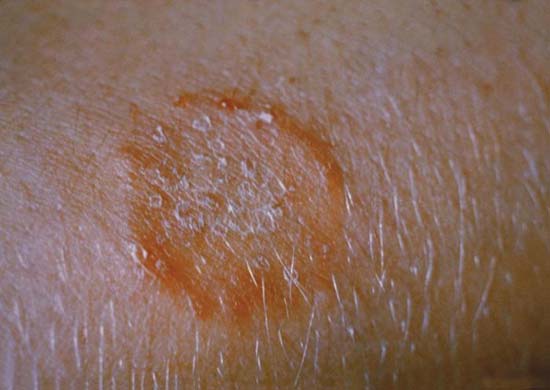
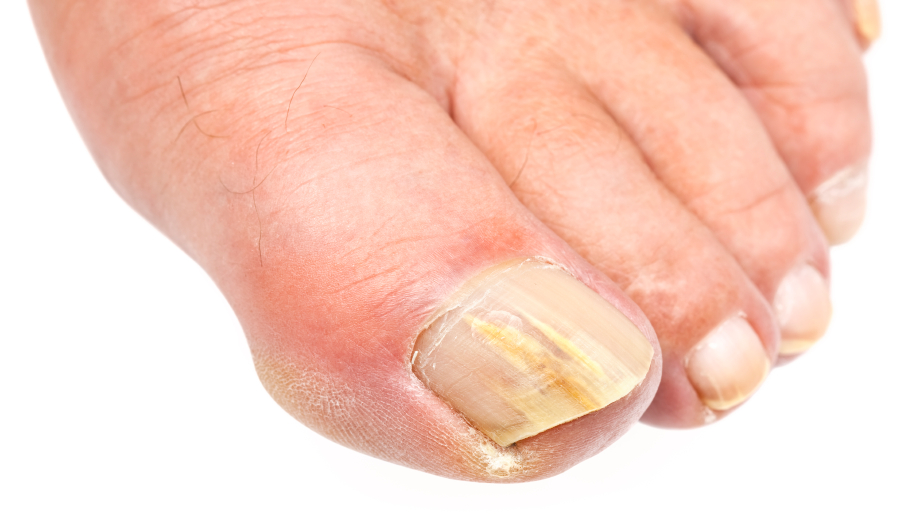
 Dermatophyte infections are also referred to as tinea. Dermatophyte infections of the skin can lead to a round, scaly rash. Because of the ringed shape of these infections they have colloquially been called “ringworm” infections. These infections are contagious. We catch them through direct contact with another person, object or animal – especially kittens. When dermatophytes infect the nails, they become thick, yellow and hard. They may eventually split or fall off. When tinea infections affect the feet or groin we refer to these infections as athlete’s foot or jock itch.
Dermatophyte infections are also referred to as tinea. Dermatophyte infections of the skin can lead to a round, scaly rash. Because of the ringed shape of these infections they have colloquially been called “ringworm” infections. These infections are contagious. We catch them through direct contact with another person, object or animal – especially kittens. When dermatophytes infect the nails, they become thick, yellow and hard. They may eventually split or fall off. When tinea infections affect the feet or groin we refer to these infections as athlete’s foot or jock itch.
Fungal skin infections may also be caused by a fungus called Malassezia furfur. These infections, also called tinea versicolor, lead to scaly patches that vary in color from white to pink to brown and are often distributed on the chest and back in a Christmas tree pattern. Tinea Versicolor tends to occur in the summers during high humidity exposures and after treatment may recur. If the skin is tanned during the infection, after treatment white patches may remain on the skin appearing as if the infection is still active. Once the tan fades, the patches typically blend in with the surrounding skin becoming less noticeable; Yet another reason to avoid the historically desirable tan and tanning salons.
Diagnosing Fungal Skin or Nail Infections
Fungal infections are diagnosed clinically by your doctor. Your dermatologist may perform a scraping of the skin to analyze the scale under the microscope. The physician may also treat empirically for what clinically appears consistent with the infection. Rarely, a skin biopsy is performed to clinch the diagnosis.
Minimize your risk of developing a yeast or dermatophyte infection on the skin by adhering to these tips:
- keep your skin dry
- keep your skin clean
- avoid direct contact with a person with a yeast or dermatophyte infection on the skin
- wear gloves whenever you are gardening
- avoid sharing personal items like nail clippers or socks
- try to lose weight to eliminate excess skin folds
Treatment
 A dermatologist may prescribe an antifungal cream or power if a yeast or dermatophyte skin infection develops. In situations where an infection covers a large area, a systemic antifungal pill may be necessary. The pills can adversely affect the liver so trials of topical agents are often preferred.
A dermatologist may prescribe an antifungal cream or power if a yeast or dermatophyte skin infection develops. In situations where an infection covers a large area, a systemic antifungal pill may be necessary. The pills can adversely affect the liver so trials of topical agents are often preferred.
Fungal infections of the nails are more challenging to cure because the topical agents cannot easily penetrate the hard nail plate. These nail infections usually require a prescription antifungal pill. An antifungal nail lacquer is also available for treating certain fungal nail infections in mild to moderate cases. Laser therapies are new non-medication methods physicians are using to eradicate toe nail fungal infections.
Despite the many treatment options for fungal infections recurrence often do occur. Some individuals may be more susceptible to these fungal infections than others. Currently, we do not have cures for these infections, however lifestyle modifications, preventative creams and powders can keep these infections away.

